
Underneath the mask of the person holding your heartbeat in their hands is one with a heartbeat all his or her own. Not God, and surely mortal, this person accepts a tremendous responsibility after entering through workplace doors, not always knowing what will arise on the other side.
Every day, surgeons deal with the fears of others — and their own, too. Stressors and a high burnout rate raise questions about why they would continue in their profession. Their job includes an immense amount of risk, yet for surgeons, it’s the reward that keeps them going.
About 450 surgeons are employed in the state of Wisconsin, according to the United States Department of Labor. And there’s a reason there are so few of them: the process of becoming a surgeon is lengthy, spanning 13 years or more. It starts with a bachelor’s degree, followed by four years in medical school, and then years of practice under supervision, or what’s known as residency. Residents who pursue a fellowship may even have another one to three years of training after that. To better understand the process, says Dylan Jacobus, a third-year resident, think about “Grey’s Anatomy” and the progression of the doctors like Meredith Grey from her first season as a resident to her current status as head of general surgery.
For 30-year-old Jacobus, a resident at the University of Wisconsin School of Medicine and Public Health, taking the plunge into an education that lasts nearly a decade and a half was all because of who he is at his core.
“I wanted to help people, ultimately, and I felt that the way my behaviors are — or the way my attitude is — and kind of the personality that I have and my interests, fit most with being a doctor,” Jacobus says.
But for other doctors, going into medicine wasn’t an easy choice, or a choice at all. Peter Nichol, a native Madisonian and surgeon, faced the prospect of going into medicine at an early age, and frankly, tried to run from it. Watching his pediatrician mother take calls in the middle of the night from patients was something he never wanted; today he’s a pediatric surgeon. He didn’t know he was the type of person “who liked to go running toward fires, at least initially,” Nichol says.
While abstract to the average eye, many surgeons see the surgeries they perform as concrete practices. They become good at what they do, yet still find instant gratification after completing an operation they do every day. It’s a foreign concept to those of us going under the knife for a life-changing surgery.
For surgeons, it’s just another day at the office.
“Today I saw four patients whose lives were tremendously improved by stuff that took me a half an hour,” says Dan Resnick, professor and vice chairman of neurosurgery at the University of Wisconsin School of Medicine and Public Health. “Being able to spend an hour in the [operating room] and have someone who’s in a wheelchair walk; I mean talk about an ego trip.”
Still, complications, stressors and unwanted outcomes remain a part of the job. Appendicitis may be a quick fix, but not all cases are that straightforward. Some operations involve a great deal of risk, and some don’t always have the best outcomes.
Sharon Weber, a surgical oncologist at UW Hospital and Clinics, has had her share of experiences with unfortunate endings. She deals in data, backing things up with fact and an understanding of biology. But as she treats her patients, she forms friendships, which makes it difficult to rationalize their sometimes incurable cases.
“I think there’s an anxiety about it, and there’s a hopefulness for [patients] having the best outcome,” Weber says. “There are times where it is just very, very difficult to deal with, when you see lots of people dying of cancer regardless of what we do.”
It’s common for surgeons to lose sleep over their patients in various ways. They spend hours in the operating room, but also lay awake at night thinking of them. The question that lingers in many minds is, “Did I do the best I could?” Jacobus talks about having imposter syndrome, which is a feeling of self-doubt, even after proven success, according to the Harvard Business Review. He’s still green in his field and finds himself questioning if he’s good enough. Even after the surgery is complete, Jacobus thinks about the patients and their recovery. If the process doesn’t go as planned, Jacobus can’t help wondering if it’s something he did.
Jim Maloney, a thoracic surgeon from UW Hospitals and Clinics, finds himself telling his residents, “You have to have a willful lack of insight, because if you’re focused all the time on the things that could go wrong, [then] you’re not going to be able to accomplish the mission at hand.”
For people who fix so much, it can be incredibly challenging to walk away from something that won’t mend. Nichol reflects on an incident in which one of his children’s classmates died; he admits that he struggled to stop working on the case.
“You at some point have to make peace with your limitations, or what you can and cannot fix, and you have to be willing to accept that, and that’s hard sometimes,” Nichol says.
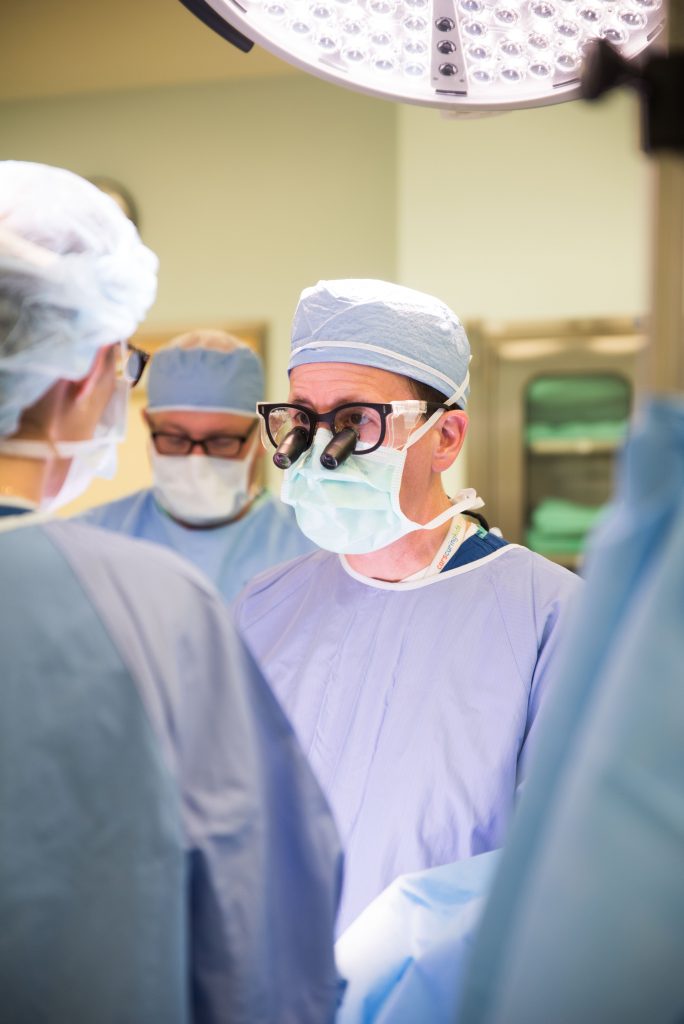
When another child came in with a similar injury, Nichol recalls being “terrified,” remembering the last four children with that kind of injury that had died. Yet, as Nichol worked through the fear and the surgery, the boy kept breathing and came out of it alive. Nichol says that to be fearless is to be ignorant. This surgery involved incredible risk, but what happened in that room — with the help of 32 other medical professionals — took courage for an immense reward: a heartbeat.
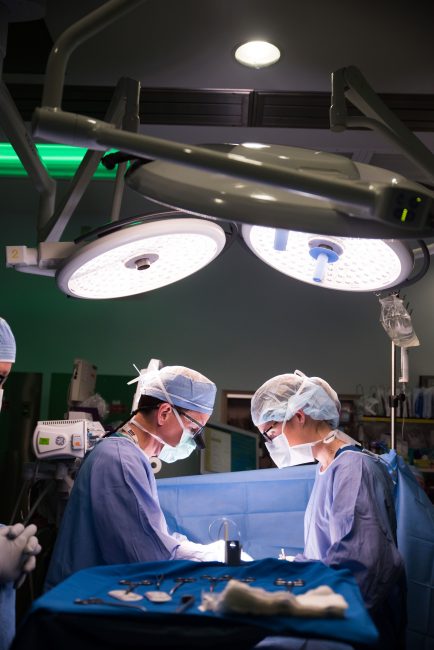
Dealing with the hardships that come with this profession isn’t something that’s always been addressed. Publications such as “Surgeon Burnout: A Systematic Review” reflect alarmingly high rates of burnout not only among physicians, but especially among surgeons: The burnout rate in surgical specialties reaches from 37-53 percent. General surgeons are among the leaders in burnout rate, with half falling victim.
This high burnout rate has raised eyebrows in the medical field and caused people to act. Medical schools, the health care system and even the curriculum taught within the schools are adjusting to accommodate more wellness practices. Gwenevere McIntosh, a general pediatrician and associate dean for students at the UW School of Medicine and Public Health, provides support to the students, from academics to counseling.
Currently, the school offers classes that integrate physician wellness into the curriculum. During the first four weeks of medical school, students plan designated time in their schedules for exercise, sleep and cooking. Within the school, there’s a “no studying” zone, where they can relieve stress through meditation or yoga. Introducing these skills early on is crucial for physicians so they can provide the best possible care. McIntosh says that in order to properly care for their patients, physicians first have to take care of themselves. Encouraging wellness for physicians in medical schools is a fairly new practice within the last five or 10 years, according to McIntosh.
Admittedly, Nichol says he doesn’t cope well with the stresses of being a surgeon. He says he finds other outlets to relieve stress, such as establishing his own foundation, “Cars Curing Kids,” which is a group of car enthusiasts who support research and programs for childhood diseases at the American Family Children’s Hospital. The stresses from being a surgeon take a toll on their bodies, too, notes Nichol, who practices yoga at home under the guidance of his physical therapist.
Weber says she deals with stress by focusing on always progressing. When she runs into challenges, she finds it easier to go in with a mindset of doing the best you can, while always trying to improve.
After knowing everything they’re up against — sleepless nights, heartbreak, burnout and risk — why surgeons keep moving forward becomes an even larger question. When asked why he continues, Maloney puts it simply: “What else would I do?” The mastery of his craft pays him in immediate gratification. For many surgeons, that’s enough.

Olivia, the editor in chief is a senior majoring in journalism with a focus in strategic communications as well as with Spanish. Upon graduation, she hopes to land a job as an editor in chief at Southern Living magazine.